Coccyx (Tailbone) Pain and Your Pelvic Floor
The connection between the coccyx and pelvic floor
How are coccyx pain and the pelvic floor connected? Could pelvic floor tension be contributing to your tailbone pain?
Many treatments for coccyx pain focus directly on the tailbone itself. However, understanding how pelvic floor function influences the coccyx may help explain why some people experience persistent or recurring pain. Pelvic floor muscle tension can sometimes contribute to coccyx pain, and coccyx pain can also increase pelvic floor tension—creating a cycle that may be overlooked.
Let’s start with the anatomy
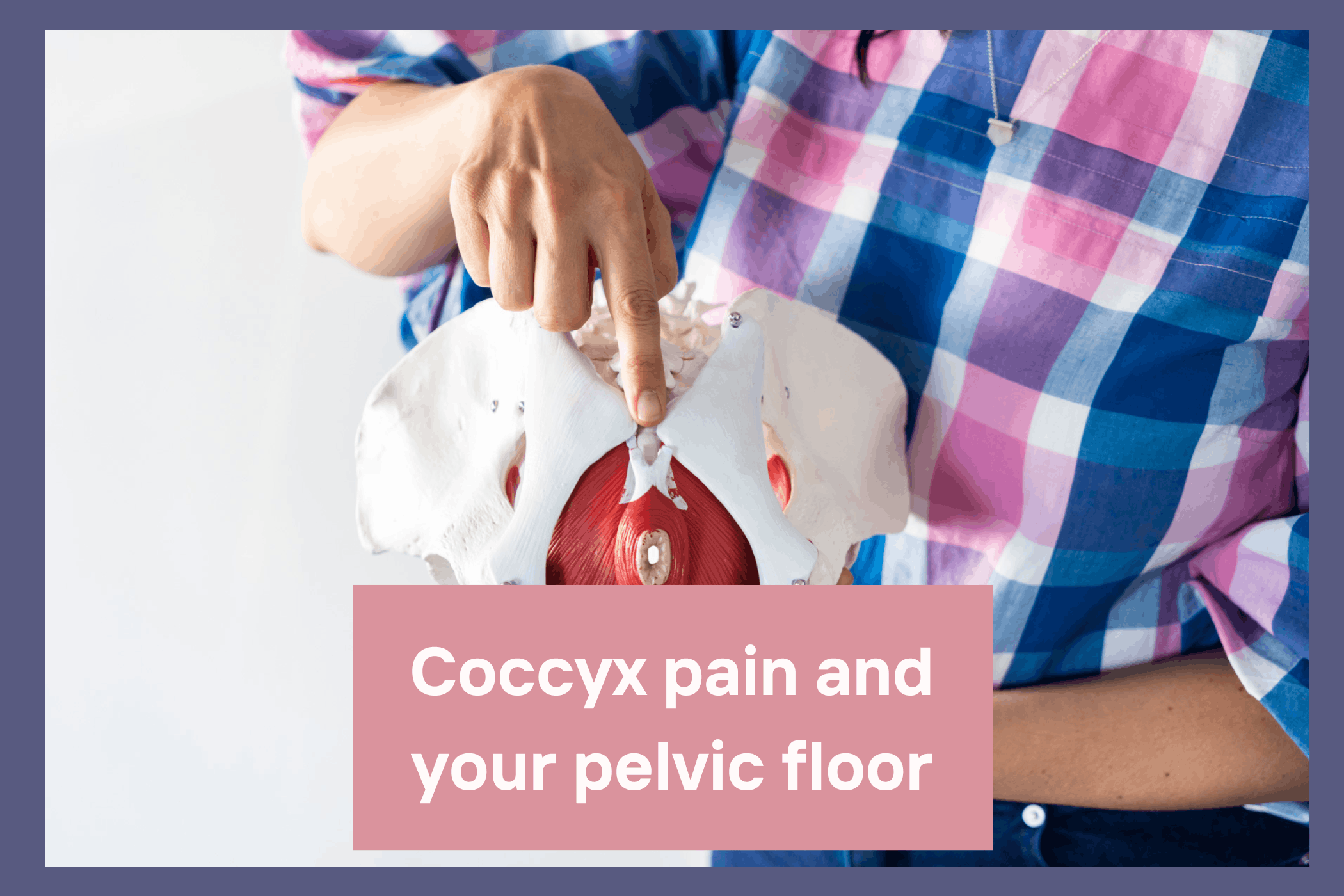
The coccyx, commonly called the tailbone, sits at the base of the spine and is made up of three to five small bones that are usually fused together. It connects to the sacrum via the sacrococcygeal joint.
Coccyx pain is often associated with falls, prolonged sitting, or changes in posture that affect how this joint moves. However, the coccyx does not function in isolation. It serves as an important attachment point for multiple muscles and ligaments, including the pelvic floor.
What is the pelvic floor?
The pelvic floor is a group of muscles and connective tissues that form a supportive sling at the base of the pelvis. It helps support organs such as the bladder, uterus, and rectum, and plays a role in continence, posture, breathing, and everyday movement.
Rather than being static, the pelvic floor is dynamic. It responds to activities like walking, sitting, lifting, and breathing, adapting continuously to support the body.
How does the pelvic floor affect the coccyx?
The pelvic floor muscles attach directly to the coccyx. When these muscles contract, the tip of the coccyx gently moves forward. When they relax, the coccyx moves slightly backward.
If the pelvic floor muscles are holding excess tension, they may place ongoing strain on the coccyx and the sacrococcygeal joint. This can influence coccyx position, movement, and sensitivity.
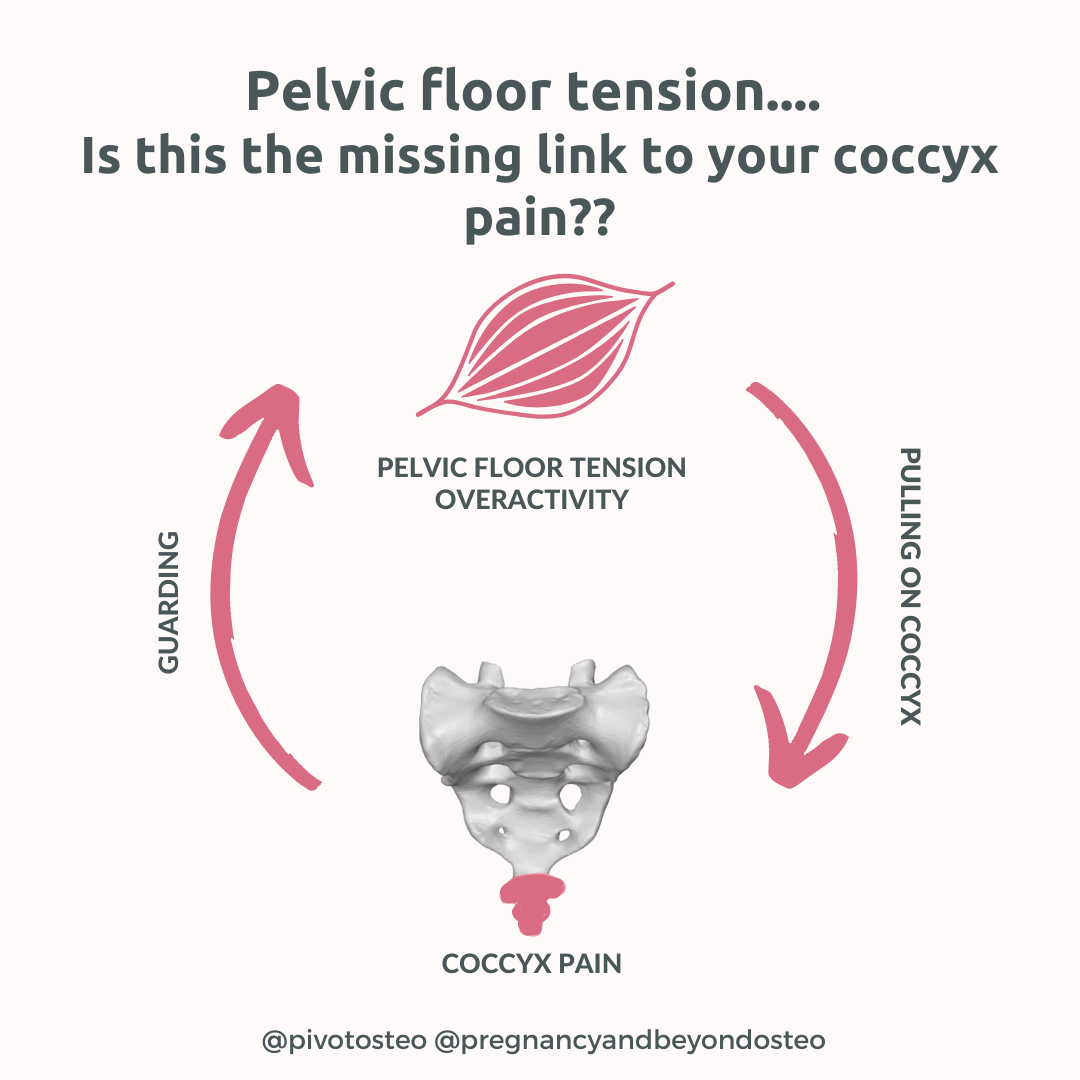
In some cases, a pain–tension cycle develops:
Coccyx pain leads to protective pelvic floor tightening
Pelvic floor tension increases strain on the coccyx
Pain persists or becomes more sensitive over time
Research suggests pelvic floor dysfunction is commonly present in people with coccyx pain. While coccyx pain is more common in women, people of all genders can be affected.
Factors such as constipation, bladder or bowel symptoms, and conditions like endometriosis may also influence pelvic floor tension and coccyx sensitivity.
What can you do?
If pelvic floor tension may be contributing to your coccyx pain, some strategies that may be helpful include:
Diaphragmatic breathing to encourage pelvic floor relaxation
Gentle stretches and mobility exercises that promote length and movement
Self-release techniques to reduce muscle tension
Stress-management approaches, as pelvic floor tension often increases during periods of stress
Assessment by a pelvic-health-trained practitioner who can look at both the pelvic floor and the coccyx
Could osteopathy help with coccyx pain?
Pelvic floor tension can be a significant contributor to coccyx pain, but it is rarely the only factor. Osteopaths take a whole-body approach, considering how posture, movement patterns, breathing, stress, and biomechanics may influence both pelvic floor function and coccyx load.
Osteopathic care for coccyx pain may include external hands-on techniques, movement guidance, lifestyle support, and—where appropriate and with consent—internal pelvic floor assessment and treatment. These options are always discussed collaboratively and are entirely optional.
If coccyx pain is affecting your comfort or daily life, a whole-body assessment may help clarify what is contributing and what support options are available.
Disclaimer: This blog is for general informational purposes only and does not constitute the practice of medicine, osteopathy, nursing or other professional health care services, including the giving of medical advice, and no practitioner/patient relationship is formed. The use of information on this blog or materials linked from this blog is at the user's own risk. The content of this blog is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Users should not disregard, or delay in obtaining, medical advice for any medical condition they may have, and should seek the assistance of their health care professionals for any such conditions.